New nationwide lung transplant scheme with urgent categories dramatically reduced waiting times for sickest patients
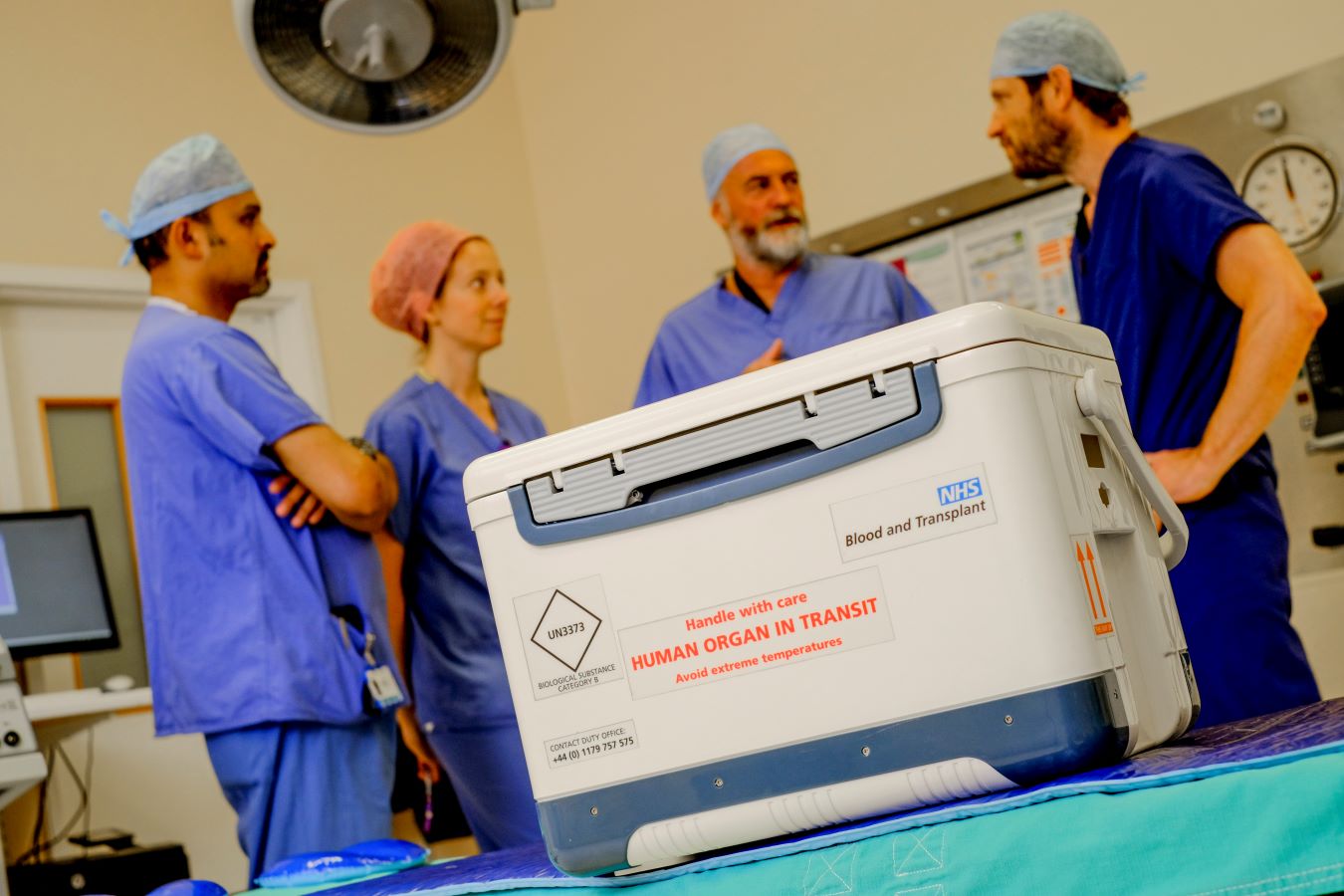 The creation of a nationwide organ transplant allocation policy successfully enabled the sickest patients to receive transplants sooner, a new research paper shows (1).
The creation of a nationwide organ transplant allocation policy successfully enabled the sickest patients to receive transplants sooner, a new research paper shows (1).
The paper shows waiting times dropped from a median of 427 days to 292 days and the odds of being transplanted within six months increased by 41%.
The updated UK Lung Allocation Scheme (UKLAS) was introduced by NHS Blood and Transplant with advice from an expert advisory group (2).
The changes to the former scheme included creating new 'Urgent' and 'Super Urgent' (3) patient categories and replacing the five geographic zones with a nationwide system.
The paper's findings
The new paper, published in the BMJ journal 'Thorax', covers 471 patients who were registered on to the waiting list between the policy’s introduction in May 2017 and January 2019 (4).
It says: "Shifting from a geographic to a clinical urgency based lung allocation scheme, prioritising the sickest patients, improved odds of transplantation with comparable waiting-list mortality and early post-transplant survival rates."
The study found people on the super urgent waiting list had a median waiting time of eight days, people on the urgent waiting list had a median waiting time of 15 days, and people on the non-urgent list had a waiting time of 585 days.
More time is needed before a full analysis of longer-term patient outcomes can be carried out. However, there was a reduction in Primary Graft Dysfunction (PGD) (5) – when the lung takes days or weeks to 'wake up' and function properly – which is good indicator that there will be an overall improvement in long term patient outcomes. The incidence of the most severe form of PGD within 72 hours of transplantation reduced significantly, from 25% to 15%.
The overall waiting-list mortality and one-year post-transplant survival rates were similar, indicating the sickest patients were still able to recover from transplants while non-urgent patients were not disadvantaged.
COVID-19 significantly reduced lung transplant activity and increased waiting times again but transplant centres are now fully open.
NHSBT constantly works to improve the allocation policies for all organs, with input from the organ-specific advisory groups, made up of transplant surgeons, patient representatives, and other members of the transplant and donation community.
Georgie's story
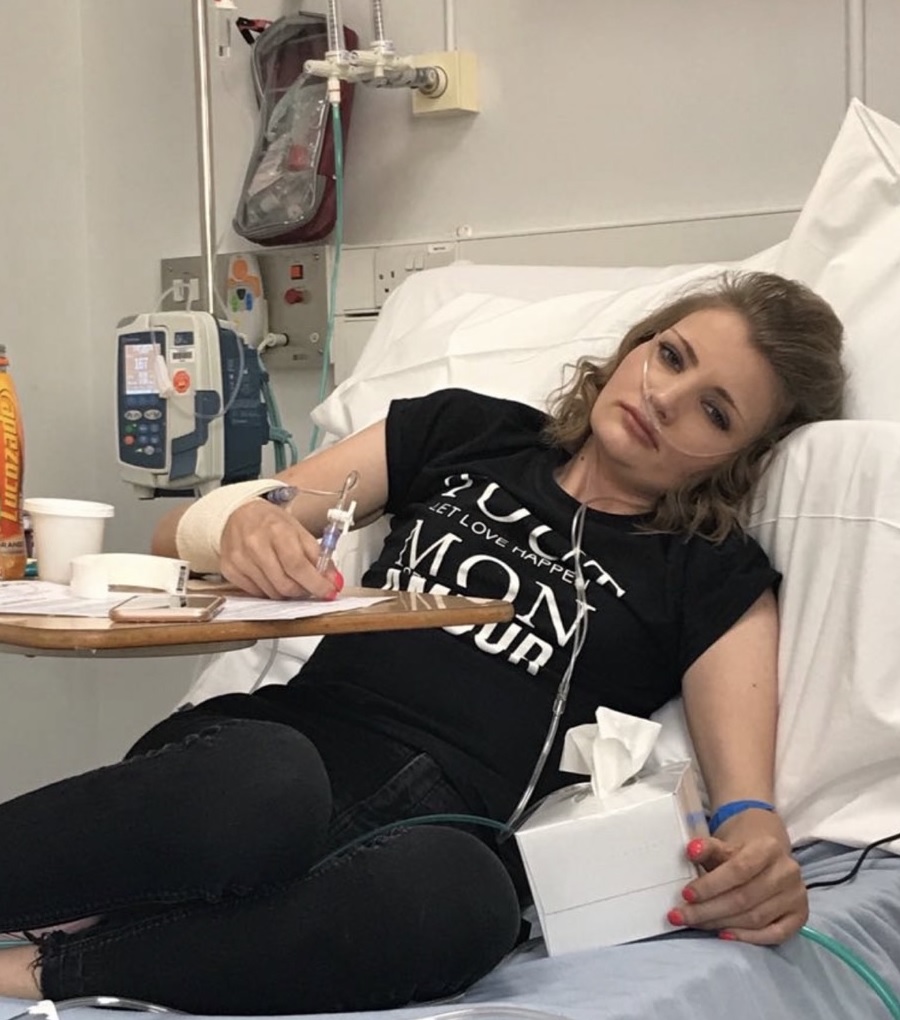 Georgie Cooper from Chelmsford received a lung transplant at Harefield Hospital in 2021 through the new 'urgent' waiting list. The 26-year-old has cystic fibrosis and by the time of her transplant she was considered to be just weeks away from death.
Georgie Cooper from Chelmsford received a lung transplant at Harefield Hospital in 2021 through the new 'urgent' waiting list. The 26-year-old has cystic fibrosis and by the time of her transplant she was considered to be just weeks away from death.
"Before my transplant I was suffocating with every breath I tried to take," said Georgie, who works for Essex County Council. "I am so happy I could be prioritised for an urgent transplant. Knowing that if you get sicker, the system adjusts, really helps. It was amazing to feel the air in my lungs after my transplant.
"I feel reborn. I am so grateful to the donor and their family, they are my heroes."
Statements
Press release notes
- Early experience of a new national lung allocation scheme in the UK based on clinical urgency article
- The new policy was introduced by NHS Blood and Transplant, with input from the Cardiothoracic Advisory Group (Lungs) which is made up of experts from the donation and transplant community.
- To be classed as 'Super urgent', patients must be receiving support with veno-venous extracorporeal membrane oxygenation (VV-ECMO), a form of mechanical life support which performs the function of the lungs that are failing. People who met certain disease-specific factors were classed as urgent.
- Later periods were not chosen to avoid the confounding impact of the SARS-CoV-pandemic, which resulted in a 48% decrease in the number of donors and a significant reduction in lung utilisation.
- Learn more about early risks of a lung transplant